Atrial Fibrillation
Atrial fibrillation (AF) is a common heart rhythm abnormality where the normal regular rhythm (‘sinus’) is replaced by an irregular and often rapid heart beat.
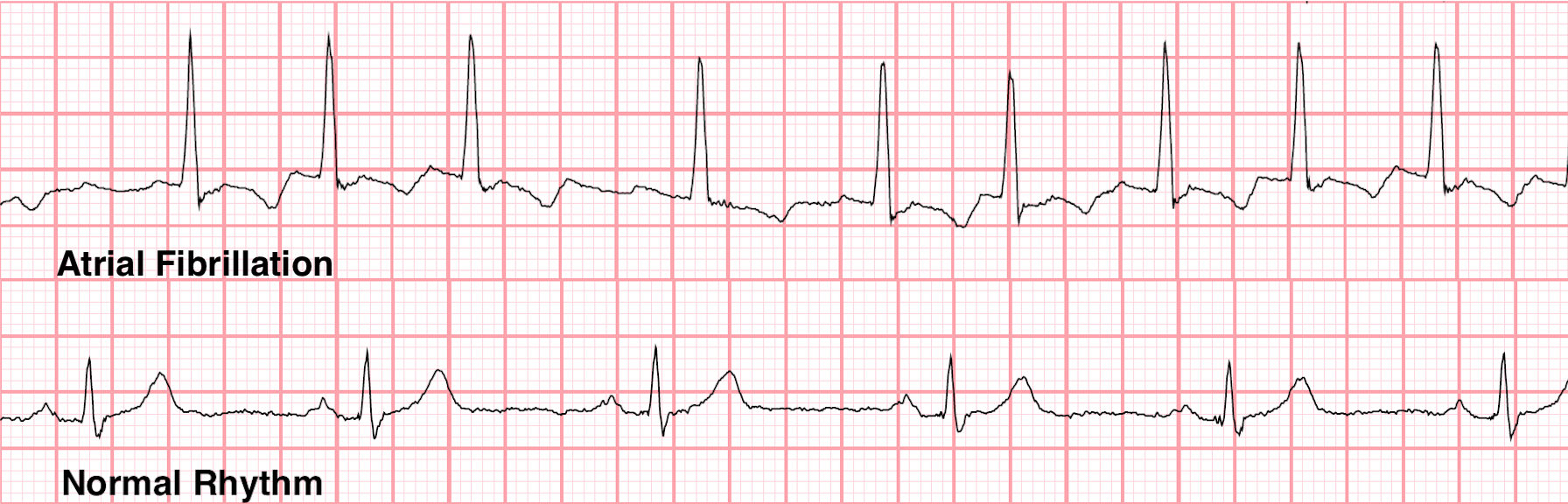
Atrial fibrillation may come and go (called paroxysmal AF) or be present most of the time (called persistent AF).
Cause
The incidence of atrial fibrillation increases with age and is more common in the setting of high blood pressure, heart disease, excess weight, obstructive sleep apnoea, and excessive alcohol intake. However, many cases of atrial fibrillation occur without an evident cause. In these cases there may be a genetic predisposition accompanied by subtle environmental factors which bring on the condition.
Consequences
In general the symptoms of atrial fibrillation are unpleasant. But some people are unaware they are in atrial fibrillation, or else symptomatic during some episodes but not others.
Whether or not symptoms occur, there is an increased risk of stroke and heart failure in atrial fibrillation.
Prevention of Stroke
Anticoagulant medications are used to prevent stroke when the risk is high. Your doctor will estimate this risk using factors such as heart failure, high blood pressure, age, diabetes, vascular disease, and previous stroke or transient ischaemic attack (TIA). When the estimated risk is high enough, an anticoagulant medication is usually recommended. Warfarin was traditionally used, but it is now more common to use a direct oral anticoagulant, which does not require the same strict blood-test monitoring. Apixaban, rivaroxaban, and dabigatran are available in Australia.
Treating Symptoms and Preventing Heart Failure
Two strategies may be used for the treatment of AF: rate control, or rhythm control.
A rate control strategy accepts the presence of AF but aims to reduce associated rapid high heart rates with medication. This method is often effective for reducing symptoms and preventing heart failure.
A rhythm control strategy is employed when symptoms remain despite adequate rate control, or when the heart rate cannot be controlled. Uncommonly, heart failure may occur despite adequate rate control, and in these cases a rhythm control strategy is preferred.
Rhythm Control with Drugs
When AF causes troubling symptoms, an attempt can be made to keep the heart in normal rhythm. This is sometimes accomplished by anti-arrhythmic medication alone, but a DC cardioversion (‘electrical shock’) may be needed to get the heart back into rhythm before medication keeps it in rhythm.
Anti-arrhythmic medications may avoid the need for an invasive procedure but are associated with side-effects of their own (see flecainide, sotalol, or amiodarone). Some recent evidence suggests that in the long term, catheter ablation is associated with a lower risk of complications compared with medication. Nonetheless, many patients are maintained in normal rhythm safely in the medium to long term on medication alone, often with few side effects.
Rhythm Control with Catheter Ablation
When medication is ineffective, not tolerated, or not preferred, catheter ablation of AF is an effective procedure for the control of atrial fibrillation.
Ablation is based on the observation that extra beats, called “ectopic beats”, originate in the pulmonary veins and are a frequent trigger for atrial fibrillation. Catheter ablation electrically isolates the pulmonary veins from the left atrium. Extra beats are no longer able to escape from the pulmonary veins into the heart.
Catheter ablation works best when the heart is healthy, and the fibrillation comes and goes. It is less effective for durably controlling persistent AF.
Summary of Management
Treatment of atrial fibrillation begins with attention to lifestyle risks. Losing weight, reducing alcohol intake, and strictly controlling blood pressure, may eliminate or reduce the frequency of attacks.
If AF continues, medication may be used or catheter ablation if preferred. Often the two treatments are used together to increase the chance of success.
If symptoms continue despite all these measures, a pacemaker will allow adequate dosing of medication or as a component of AV node ablation.
At any stage of the treatment process, a decision may be made to adopt a rate control strategy, accepting that the symptoms of atrial fibrillation often reduce over time, and the risk of further intervention is not warranted.
Importantly, the symptoms of AF can almost always be controlled and most patients enjoy a good quality of life with few or no limitations.
